HIGHLIGHTS
Placenta Accreta Spectrum (PAS) Program of Excellence
Leads:
- Fatima A. Estrada Trejo, MD Director, PAS Center
- Lance R. Bruck, MD, Executive Vice Chair, Strategic Development, Obstetrics & Gynecology and Women’s Health
- Pe’er Dar, MD, Vice Chair, Obstetrical Ultrasound & Fetal Medicine
- Patrick F. Timmins, MD, FACS, Vice Chair, Legislative Affairs, Obstetrics & Gynecology and Women’s Health
Placenta accreta spectrum disorders (PASDs) are life-threatening obstetric conditions characterized by abnormal placental adherence or invasion into the uterine wall. The disorders are historically divided into three types:
- Accreta: abnormal placental adherence
- Increta: invasion of the placenta into the uterine wall
- Percreta: penetration of the placenta through the uterine wall into surrounding tissues
The Montefiore Einstein PASD Program of Excellence provides comprehensive care from diagnosis through postpartum recovery, leveraging a multidisciplinary team and advanced protocols to optimize outcomes for these surgically complex disorders that can be life-threatening for women who are pregnant.
As a regional perinatal referral center, we get referred these cases because we have the appropriate personnel, including high-risk obstetricians, skilled and experienced gynecologic oncologists (often the surgeons resecting and reconstructing the patient’s organs), vascular surgeons, urologists (the placenta often grows into the bladder or obstructs one or both ureters), obstetric anesthesiologists, as well as an experienced blood bank team and, of course, the fantastic and experienced Montefiore Einstein Nursing team. Most general obstetrician/gynecologists have neither the expertise nor the resources of a system that has the necessary structure and redundancy to handle the complexities of these cases. Not long ago, Montefiore Einstein also did not have such redundancy, and we had some poor outcomes that led to some community relations challenges. Montefiore Einstein leadership recognized the gap and invested in new leadership to overcome these challenges that are affecting the Bronx community.
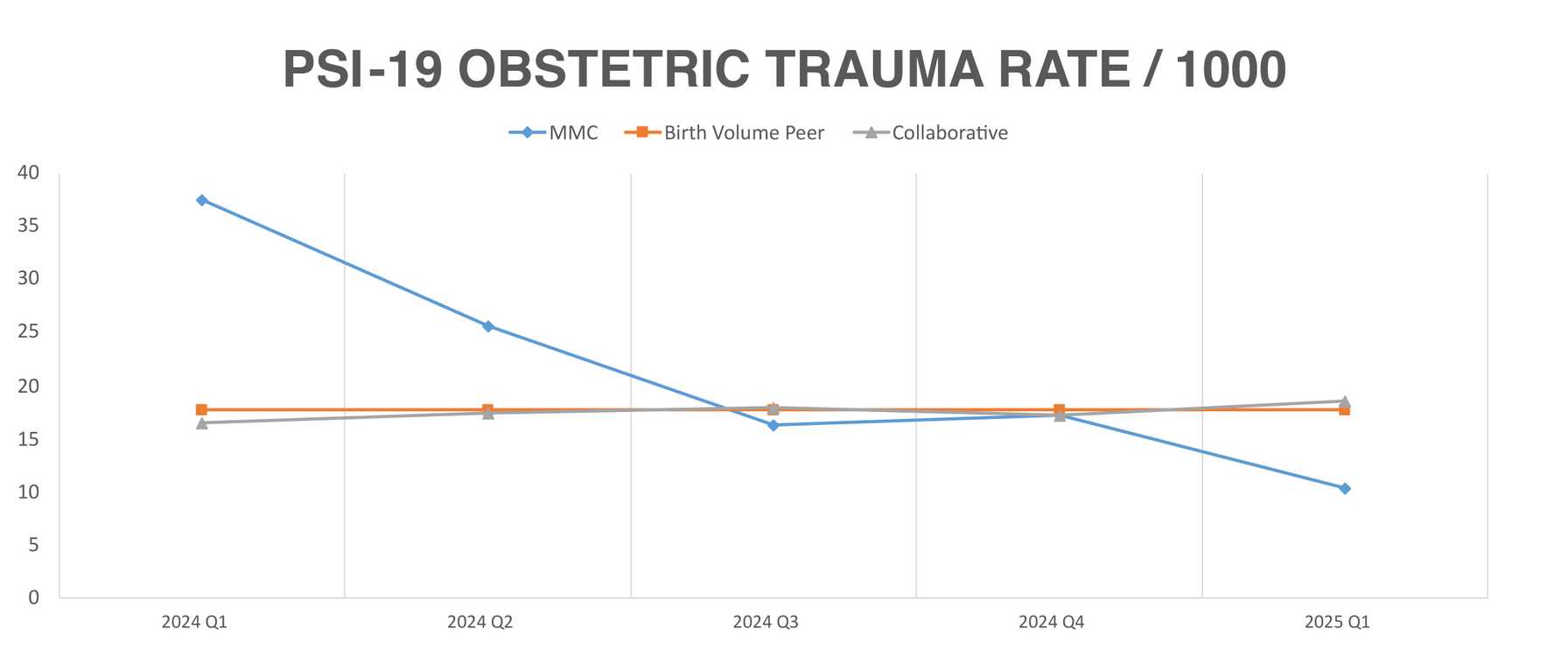
Since reorganizing and restaffing with experienced expert surgeons, our obstetric trauma rates have dropped precipitously (Figure 1). We have had 18 patients with this syndrome since September 2024, and all 18 had better than average outcomes for complications, transfusions and all other metrics of good surgical outcomes.
We intend to become known as the center delivering the highest standard of multidisciplinary, evidence-based care for patients with placenta accreta spectrum disorders, while advancing research, education and advocacy to improve maternal outcomes and reduce morbidity and mortality associated with PASD. In our three-to-five-year plan, we plan to become a national leader in the diagnosis, management and innovative care of PASD, fostering a model of excellence that integrates clinical expertise, cutting-edge research and compassionate, patient-centered care. We are moving from a reactive institution that could not handle these situations to one of the best in the country. More importantly, having a program like this best serves the needs of the Bronx, where risk factors for these conditions remain very high (e.g. prior cesarean delivery).
Program Overview
Core Services
1. Diagnosis
- Risk stratification: based on history (e.g. prior cesarean sections, placenta previa)
- Advanced imaging:
- High-resolution transvaginal ultrasound with color Doppler
- Magnetic resonance imaging (MRI) for complex or posterior placentation
- Multidisciplinary case review: weekly imaging and surgical planning conferences
2. Multispecialty Management
- Maternal-fetal medicine (MFM): leads care coordination and delivery planning
- Obstetric anesthesia: preoperative optimization and intraoperative management
- Gynecologic oncology and pelvic surgeons: for complex resections
- Urology and interventional radiology: for bladder involvement and embolization
- Critical care and transfusion medicine: hemorrhage protocols and intensive care unit care
- Neonatology: Level IV neonatal intensive care unit for preterm or compromised neonates
- Mental health and social work: perinatal mental health and family support
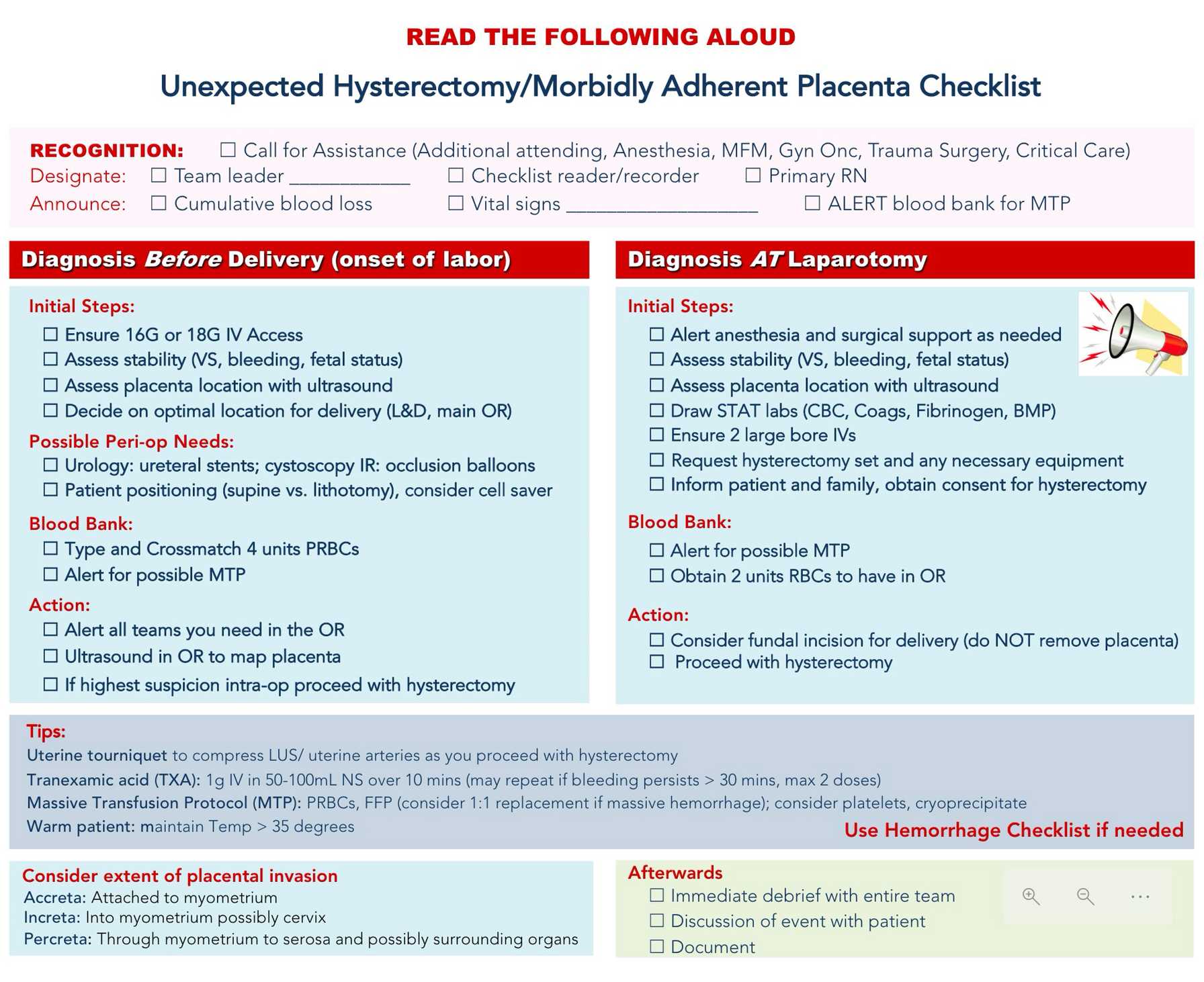
3. Delivery Protocols
- Planned cesarean hysterectomy at 34 to 36 weeks gestation with placenta left in situ
- Massive transfusion protocols and cell salvage available
- Hybrid operating room access for real-time interventional radiology
- Obstetric intensive care unit for immediate postoperative monitoring
Management Algorithm (Simplified)
- Suspected PASD: refer to PAS Center
- Confirm diagnosis: imaging and risk assessment
- Multidisciplinary planning: delivery at Level III or IV center
- Scheduled delivery: cesarean hysterectomy with or without interventional radiology or urology
- Postpartum care: intensive care, mental health, and fertility counseling
Research Initiatives
- Development of an institutional database for research
- National Institutes of Health funded studies on PAS pathophysiology and uterine scarring
- Biospecimen repository for molecular and genetic studies
- Clinical trials focused on conservative management and uterine preservation
- Collaboration with the Pan-American Society for Placenta Accreta Spectrum (PAS²) for multicenter data sharing
- Community-based educational initiatives to increase awareness
Education and Training
- Fellowship rotations in PASD management for maternal-fetal medicine and OB/GYN residents
- Simulation-based training for hemorrhage and complex surgical scenarios
- Annual symposium highlighting PASD innovations and outcomes
- Patient education materials and support groups
Quality and Outcomes
- Benchmarking against national PASD registries
- Morbidity and mortality reviews for continuous improvement
- Use of patient-reported outcomes to guide holistic care
Management Algorithms (Detailed)
Patient referrals
At Montefiore Einstein Obstetrics & Gynecology and Women’s Health, we know that providing patients with the best possible care includes teamwork and trust. We work closely with our valued referring physicians to ensure open communication and reliable expertise.
Contact us
Linda Gillespie, MSEd, MBA
Director, Patient Experience, Access and Special Projects, Obstetrics, Gynecology and Women’s Health, Montefiore Einstein
LGILLESP@montefiore.org