HIGHLIGHTS
Cervical Cancer Screening Performance Improvement: Self-Screening in Nontraditional Medical Settings
Leads:
- Mark H. Einstein, MD, Chair, Obstetrics and Gynecology and Women’s Health
- Michael P. Jones, MD, Chair, Emergency Medicine
- Lance R. Bruck, MD, Executive Vice Chair, Strategic Development, Obstetrics and Gynecology and Women’s Health
- Benjamin W. Friedman, MD, Quality Assurance and Performance Improvement, Emergency Medicine
- Juan Diaz Quinones, MD, Vice Chair, Operations and Integration
Project Rationale and Background
The incidence of cervical cancer is disproportionately high in the Bronx, largely due to inadequate prior screening. Nationally, approximately half of individuals diagnosed with cervical cancer have had no or limited screening follow-up, representing missed opportunities within the fragmented U.S. healthcare system. Self-sampling is a novel screening approach in the United States that enables cervical cancer screening in nontraditional settings, such as emergency departments, for individuals with limited access to care. Such approaches are now routine in Western Europe, Australia, and New Zealand.
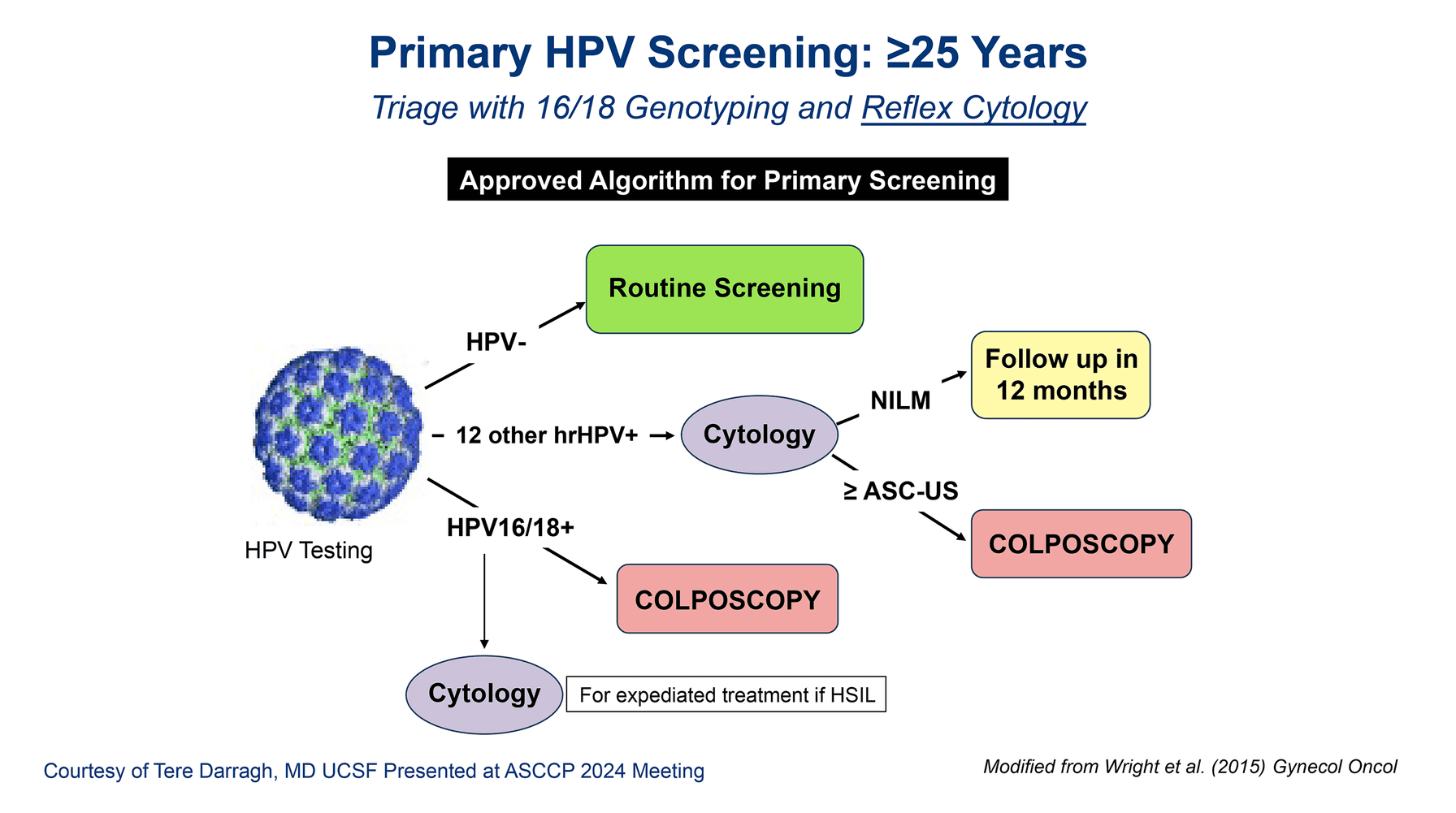
The American Cancer Society and the United States Preventive Services Task Force have updated recommendations supporting primary human papillomavirus testing for cervical cancer screening (see Figure 1 for the algorithm). Montefiore Einstein is a lead institution working to achieve U.S. Food and Drug Administration approval of self-sampling for home use, which is currently approved only for office-based use.
A critical unanswered question is whether individuals who self-sample in nontraditional settings can be successfully routed to appropriate follow-up care, such as colposcopy, after a positive test result. This information is essential for broader implementation of office-based and home-based self-sampling strategies.
In collaboration with Emergency Medicine leadership and Obstetrics and Gynecology and Women’s Health leadership, this initiative will screen individuals who present to the emergency department for unrelated conditions and have no documented cervical cancer screening. Eligible participants include individuals with a cervix who have no documented or self-reported screening within the past three years.
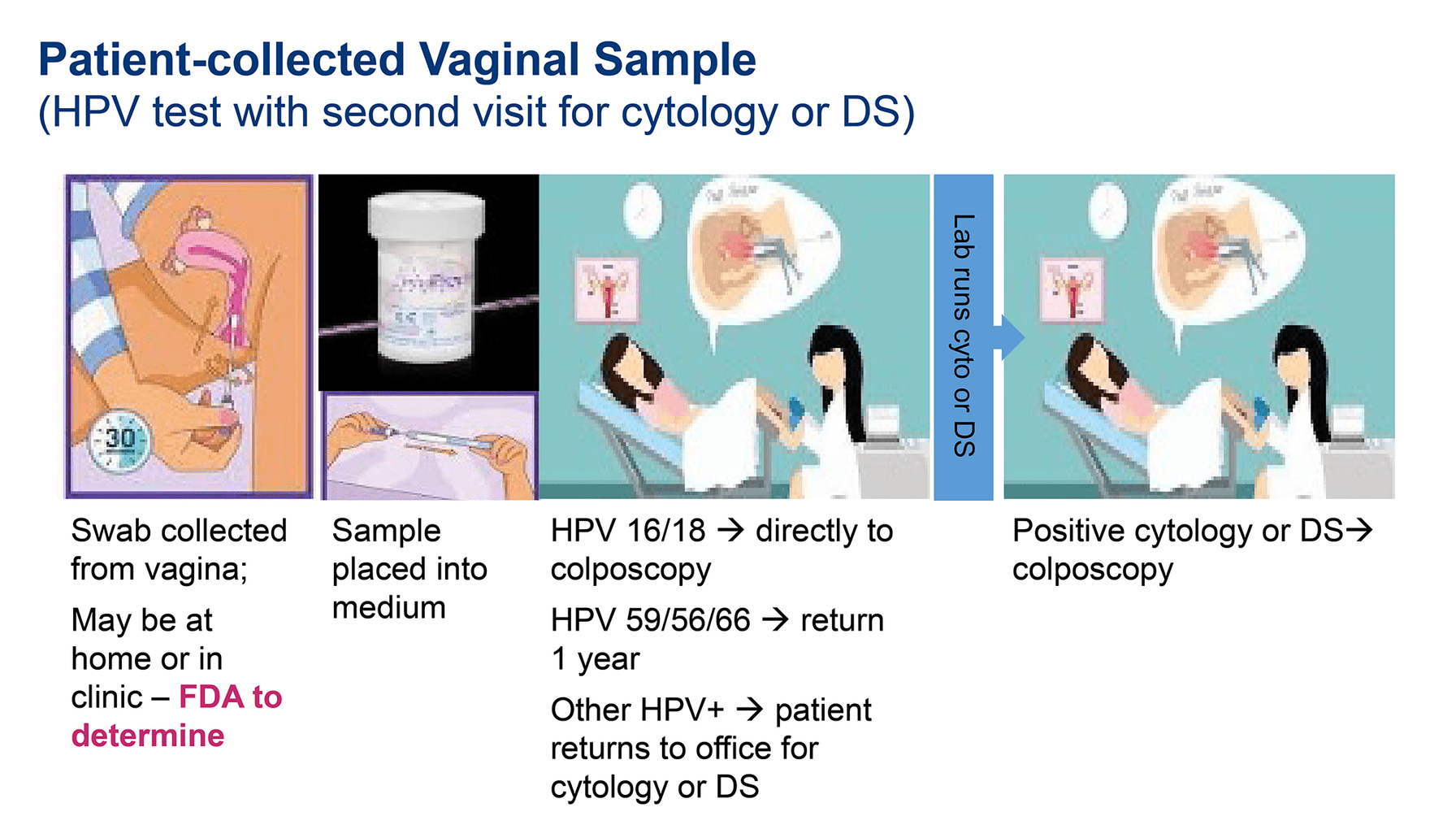
Self-sampling will be conducted in a bathroom setting concurrent with routine urine collection for other testing, such as pregnancy screening (see Figure 2 for the low-literacy visual aid used). For individuals with a positive HPV result, the Obstetrics and Gynecology and Women’s Health Department will triage results and contact patients to arrange appropriate follow-up care based on HPV subtype.
Open Issues
- Development of a data tracking system to measure program effectiveness, with a particular focus on completion of follow-up care
- Establishment of internal workflows to identify individuals who screen HPV positive and route them to care. Key metrics include the percentage of HPV-positive individuals who:
- Are successfully scheduled for follow-up care
- Present for care, such as repeat co-testing or colposcopy
- Mitigation of financial barriers that may prevent uninsured patients from accessing follow-up care, including development of an intermediary financial navigation step
- Collaboration with information technology teams to implement tracking systems that monitor:
- Successful booking of follow-up care
- Completion of indicated colposcopies
Figure 1. Algorithm for triage of care after primary HPV screening.
Figure 2. Example of low-literacy materials for self-sampling.
Patient referrals
At Montefiore Einstein Obstetrics & Gynecology and Women’s Health, we know that providing patients with the best possible care includes teamwork and trust. We work closely with our valued referring physicians to ensure open communication and reliable expertise.
Contact us
Linda Gillespie, MSEd, MBA
Director, Patient Experience, Access and Special Projects, Obstetrics, Gynecology and Women’s Health, Montefiore Einstein
LGILLESP@montefiore.org