HIGHLIGHTS
Clear Eyes. Full Hearts. Can’t Lose
In January 2025, the Department of Urology launched a six-month coaching program to address a challenge that has tested physicians for decades and intensified in recent years: burnout. Professor and Vice Chair Nitya Abraham, MD, invited Andrew Mancall, MD, a physician and executive coach, to bring a fresh approach to supporting residents through the rigors of training.
You began as a doctor. What led you to become a coach?
During my time as Chair of Radiology at Maine Medical Center in Portland, I was mentoring younger doctors and working with physicians who were burning out and under a lot of stress. I became deeply involved in physician health and was working with coaches. I didn’t really know a lot about what they were doing, but the results were impressive. To further explore this, I engaged a coach myself to experience this firsthand, and it was a great experience. This inspired me to pursue coaching as a next career step. My focus is mainly physicians, but I work with others in the healthcare industry as well, because burnout is just so endemic across what we all do.
What is fueling that burnout?
I think a lot about how the human element of what we do as physicians has been driven out of our jobs. When I was an intern, I spent 95 percent of my time with my patients. When I work with resident physicians, particularly the younger ones, they might be spending 90 percent of their time in front of computer screens documenting, which is obviously important for good patient care. But it takes them away from working with people and the caring aspect of what we do as doctors, which is so very important. COVID was also a catalyst, making this many times worse. We now recognize the impact that burnout has—not only on the individuals who are caring for patients, but the downstream effect on the patients themselves.
What brought you to the department and motivated this pilot program?
I was working with a couple of faculty members as a coach and was introduced to Dr. Abraham, who was very interested in physician well-being. She had an IRB-approved study around resident wellness in the works, but this was looking at the impact of mentoring. I suggested that we could plug in coaching for that component and maybe achieve something that would be more generalizable across all residencies.
What makes coaching unique relative to other types of support?
Coaching is really about helping individuals come to understand and accept their current life situation and move from there to a desired future state. It is driven by the desires of the individual. Something like psychotherapy is looking at psychological harm—things from the past and attempts at healing. And if I was mentoring someone, I might be suggesting things that I think they should try, which is not what coaching is about.
There is literature that suggests change sticks when people understand where they are, where they want to get to, and come to those decisions and processes themselves. That’s the real
How was the pilot program and its associated study structured?
I recruited a bench of professionally trained coaches to work with me. We had a total of six coaches, including myself. We began by giving the residents the Maslach Burnout Inventory (MBI). It’s a standardized test that’s been well vetted. All departmental house staff were invited to be part of the study. Ultimately, we had 13 residents—PGY1 through PGY5—participate. Each resident underwent six coaching sessions, once a month for six months. And then the tool was readministered, and comments were also collected.
What’s next for the coaching study?
We have submitted an abstract to the upcoming annual meeting of the American Urological Association. And then we’re talking about journal submission and where to go with that. I give Dr. Abraham big kudos for getting this done. It’s a very important study because there isn’t much literature on this yet. I believe coaching can be a very useful tool to increase physician resilience and wellness, and I think this study will potentially demonstrate that.
Coaching acted as a mix of mentorship and therapy, which is exactly what I needed when the opportunity came. It provided a space to think about how I could improve as a resident and physician, process personal and workplace issues, and gain perspective.
Samuel Yim
PGY2
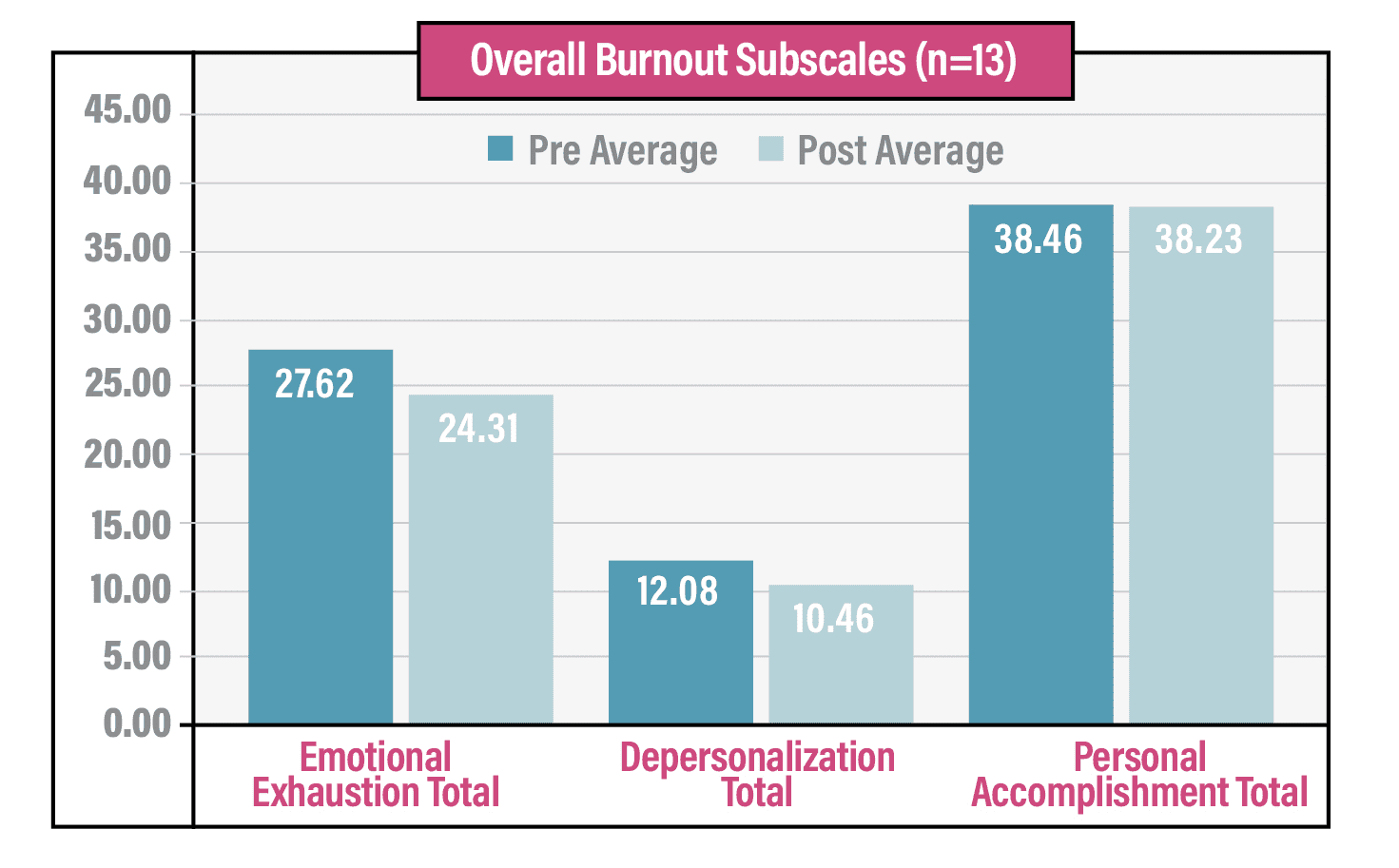
Initial Study Findings
Our analysis showed that regular professional coaching over a six-month period reduced emotional exhaustion and feelings of depersonalization, especially among PGY3 residents. Providing time for self-reflection and goal-setting through coaching could be a novel strategy for reducing resident burnout.
Patient referrals
At Montefiore Einstein Urology, we know that providing patients with the best possible care includes teamwork and trust. We work closely with our valued referring physicians to ensure open communication and reliable expertise.